The more experience I have gained working with clients, the more I have learned how much digestion plays a role in body composition, not just overall health and wellbeing. Show me someone with digestive issues, and I can show you someone who will never look the way they want to look. However, digestion is freaking complicated, and often misdiagnosed or broad brush labeled as IBS (Irritable Bowel Syndrome). So before going further, I want to clarify that I am not offering medical advice in this article, and you should always consult with your physician.
I want to dive into an actual client case and her struggle with her diagnoses’, GERD (Gastroesophageal Reflux Disease.) GERD occurs when stomach acid frequently flows back into the tube, connecting your mouth and stomach (esophagus.) So simply put, GERD occurs due to frequent acid reflux. Over time this can become a huge issue. If not addressed, this chronic inflammation can cause damage to your esophagus such as developing Barret’s Syndrome or even esophageal cancer. And not only does chronic GERD cause esophageal issues, but the inflammation can travel down into the digestive tract, also causing IBS. It needs to be taken seriously.
RECENT: Get Your Head Out of Your Arse
A new client came to me expressing digestion issues that started occurring over the last few months and how it severely impacted her appetite, and obviously comfort. She was experiencing symptoms of heartburn, a sensation of a lump in her throat after meals, and no appetite. She went to the doctor and they diagnosed her with GERD and told her to take Prilosec. Prilosec is a common antacid recommended by many physicians for GERD, however, with more and more research, this has shown to typically make issues worse over time and simply serve as a temporary Band-Aid. Antacids are potent drugs, and while many can be found over the counter, they are not safe to take long-term and can cause permanent damage to our digestive system.
The issue is, the vast majority of people who have GERD or heartburn-like symptoms are experiencing it because of LOW stomach acid, not HIGH stomach acid. So you might be asking, “Well, if GERD is caused by too little acid in the stomach and not enough, why do antacids provide temporary relief?” Great question! That is because the antacid is treating the acid reflux SYMPTOM, not the CAUSE. Like I mentioned above, it is merely a Band-aid. Symptom relief does not mean the CAUSE is being addressed! We have to remember, western medicine focuses on alleviating symptoms, not treating causes. Sorry, but it’s true. So, what happens when our stomachs produce too little stomach acid? For one, we have bacteria overgrowth. This is bad news bears for the health of our stomach lining and intestines. Second, we can’t absorb carbs very well, so most people with GERD are told to go on low carb diets, which THEN leads to chronic thyroid downregulation. So again, NOT solving the problem, just covering up a symptom to then create another problem. Bacteria overgrowth and carb malabsorption (gas) added together cause an increase in intra-abdominal pressure, which is the reason for acid reflux in the first place.
So, if this is widely understood (it is) by physicians, then why are antacids prescribed so much? Drugs for acid reflux are an insane money maker for pharmaceutical companies. Antacids are the second to highest selling drug in our country after Lipitor – which is a cholesterol medication. And as you now know, antacids don’t actually FIX or CURE anything. They are prescribed because it makes pharm companies a shit ton of money. Do I have your attention now?
Now, this is also another theory that GERD is not caused strictly by low stomach acid, but a malfunction of the lower esophageal valve, or LES. If the LES is working properly, how much stomach acid we have is irrelevant. The acid will not make it back up into the esophagus anyways. But if the LES is malfunctioning, you can experience acid reflux which therefore causes damage to our esophagus. If this is the case, wouldn’t it make more sense to focus on WHY the LES is malfunction versus trying to control stomach acid? See what I mean by digestion is complicated? Sometimes, medicine focuses on the wrong thing.
However, let’s say someone is experiencing GERD due to low stomach acid. What can they do about it? I am going to use my client as an example here. After receiving her info about her GERD diagnoses and being prescribed Prilosec, I suggested a different direction. To note as well – as a coach, I have to respect my scope of practice and boundaries. Coaches are not doctors unless they are doctors. Therefore, I reached out to a few colleagues to get their input, and I sent her peer-reviewed literature on the topic so she could make an educated decision herself. After that, I recommended taking Betaine HCL with Pepsin and dropping the Prilosec. Betaine HCL/Pepsin is an over the counter supplement that helps rebuild stomach acid to normal levels. Rather than reducing stomach acid, it supports stomach acid. After only five days of taking Betaine HCL/Pepsin, my client not only experienced significant relief, but her bloating decreased as well. Her comparison picture below says it all.
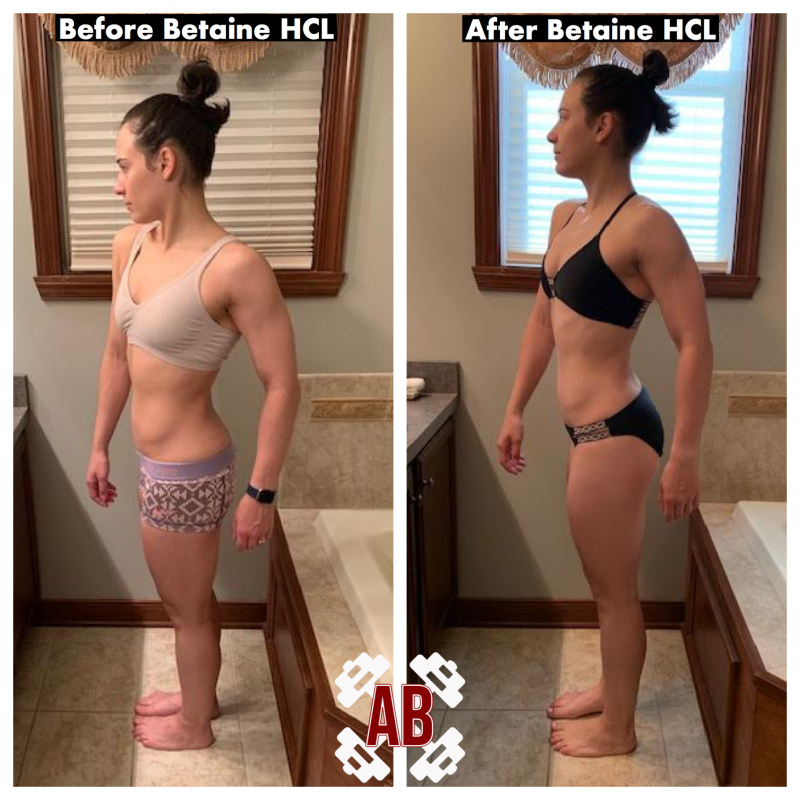
But this is just a step. We still need to figure out the WHY. Why did this just start occurring for her? Was it food intake? Stress? Is it genetic? While the Betaine HCL/Pepsin is helping to heal her gut right now, we still need to make sure there isn’t an underlying issue. If the underlying issue is addressed, she shouldn’t need to take Betaine forever. That is the goal here.
In short, this article is not intended to shoot down the medical community, but simply to encourage critical thinking, doing your research, and asking the right questions. We are our best advocates for our health, and it is on us.











Thanks for reading! And for sure it truly can be caused by a number of things. And yep, PPI's. "Anatacids" for us common folk ;-)