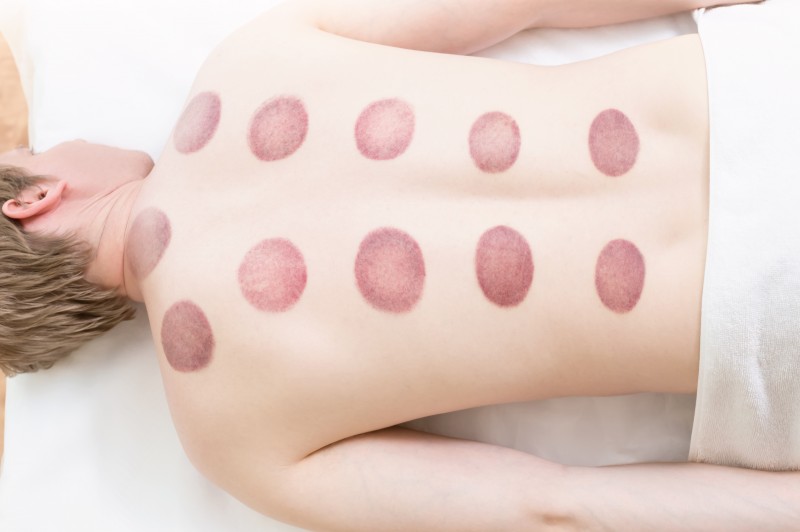
Things that once were cool tend to come back in fashion. For example, mom jeans used to be great, then they were awful, and now everyone over the age of 16 is sporting a pair. Similarly, in high school, hickeys were cool to some people, then they grew up, and they became taboo.
However, now they are back in fashion with the strength and performance world. And this isn’t just any hickey; it’s a hickey from something called cupping. So, what is this cupping stuff, how does it work, and is it just another fad?
RECENT: You Can't Out-Train Processed Foods
WTF is cupping?
Cupping is an ancient methodology that’s been used since the times of the ancient Egyptians1, 2 to cure just about anything and everything.3 However, it recently regained polarity as a recovery technique when Michael Phelps jumped into the Olympic swimming pool in 2016.
Those using cupping for rehab and recovery believe that the suction pulls the skin away from the muscles and that this increases blood flow to the area to improve recovery. Cupping is now done by a vast number of athletic trainers, physical therapists, and chiropractors as a type of decompressed myofascial tension release. However, it is believed by many scientists to work as a placebo effect.4, 5
While there are many types of cupping, the most popular are wet and dry6 with dry being most commonly used amongst the strength sports. With dry cupping, glass or plastic cups are applied to the skin with suction. Due to the negative pressure created by applying the cup with suction, your skin draws up into the cup.3, 7 These cups are left in place for about 10 minutes, and during this time, one can remain stationary.

Andriy Popov © 123rf.com
You can also have the “cupper” slide the cups up and down, or you can go through a series of exercises while the cups remain stationary. Some people say this feels like a nice stretch, whereas others say in areas of lots of muscle tension it creates a pinching sensation. Once the cupping session is done, the cups are removed, and you are sent on your way, often covered in purple circles.
Athletes who get cupped often report feeling like whatever area getting the treatment feels better and less gunky. Some practitioners use cups to remove toxins and their patients/clients report feeling cleansed.
Although athletes rave about it and western practitioners have been using it since the 1900s, skeptics claim the science supporting its application is lacking, which begs the question: Is the benefit of cupping on recovery and inflammation sufficient to justify walking around covered in circular bruises?
Suction isn’t that sucky
As stated above, the suction from cupping pulls the skin into the cup. Suction as a modality to improve healing by increasing blood flow to an area has been used since the 19th century.8 Additionally, the use of negative pressure has been put into practice as a way to improve wound healing.9-11 Hence, the use of suction to create negative pressure is the basis behind the concept that dry cupping is a recovery tool. Let's dig into understanding that.
As the cup is applied, it creates a localized negative pressure that compresses the skin at the cup rim while distracting the skin and tissue below the cup. The size and pressure of the cup determine if the distraction effect reaches the underlying muscles, hence pressure differential between the skin and underlying blood vessels causes immediate vasodilation and increased blood to the area12, 13. It’s believed that increasing blood flow to an area can be a good thing for relieving myofascial pain.
RELATED: Understanding Groin Injuries: A Muscle Tear
melpomen © 123rf.com
What about the bruising?
The negative pressure doesn't just lift then skin; it also causes bruises. The pressure reduction created by the cup can cause the small blood vessels under your skin to expand due to the now-higher pressure inside them. When the pressure difference is such that the pressure within the blood vessel is significantly greater than outside, they burst, and blood pools under the skin. When your blood pools under the skin, you get a bruise.
At first, bruises are red because lots of fresh blood is pooled under the skin, but as the days go on, the blood loses its oxygen and appears blue-black-purplish. Five to ten days post-bruise, your body makes compounds to breakdown hemoglobin, and the bruise turns a yellow-green before browning and fading.
While a lot of cupsters (my term for hipsters who cup) will tell you that the color of your marks show you how healthy of a person you are we know that the color is a reflection on the amount of blood in the area, and the amount of damage inflicted. This idea that the lighter your mark, the healthier you are, and the darker your mark, the more toxins you hold, isn’t backed by science.
Instead, what’s supported by science is the idea that when the body removes hemoglobin, it uses an enzyme known as heme oxygenase-1 (HO-1), which converts heme into biliverdin, carbon monoxide, and iron. HO-1 itself has anti-oxidant, anti-inflammatory, and pro-regenerative properties.3
So, cupsters, that color is more likely the result of:
- The extent of burst blood vessels
- How quickly that pooled blood is broken down and eliminated
- The extent of capillary ruptures verse leakage elicited from the cupping treatment
Should I cup?
When scientists looked through over 200 cupping articles this year and summarized what’s currently known about cupping and its effects. The most repeated and frequent finding was that cupping can reduce skin stiffness, inflammation, and pain.4 Over recent years, more studies have been published to substantiate that cupping can be beneficial, but some claim these studies are conducted with bias.
Overall, cupping seems to be useful for a variety of conditions and appears to work by pushing blood flow into an area and triggering a cascade of events during bruising that may be anti-inflammatory and regenerative.14 Additionally, according to science, cupping is most effective when combined with other therapies. Stepping away from the science, most people who try it out seem to feel like it works. I’ve seen cupping work great as a recovery tool to help athletes who require myofascial release.
READ MORE: If I Don't Have a Practitioner, Where Do I Go For Help?
In fact, when cups are applied to an area that requires myofascial release, and suffering muscles are taken through a range of motion exercise with the cups in place, I’ve seen it work well in reducing pain and “de-junking” a junked-up area.
So my thoughts: Try it if you have an area that requires myofascial release. The biggest downside is walking around covered in cupping hickeys.
References
- H, W. & Bs, O. A Pilot Study of Clinical Measures to Assess Mind-Body Intervention Effects for those with and without PTSD. Alternative & integrative medicine 2, 116 (2013).
- Christopoulou-Aletra, H. & Papavramidou, N. Cupping: an alternative surgical procedure used by Hippocratic physicians. Journal of alternative and complementary medicine 14, 899-902 (2008).
- Lowe, D.T. Cupping therapy: An analysis of the effects of suction on skin and the possible influence on human health. Complementary therapies in clinical practice 29, 162-168 (2017).
- Al-Bedah, A.M.N. et al. The medical perspective of cupping therapy: Effects and mechanisms of action. Journal of traditional and complementary medicine 9, 90-97 (2019).
- Ahmadi, A., Schwebel, D.C. & Rezaei, M. The efficacy of wet-cupping in the treatment of tension and migraine headache. The American journal of Chinese medicine 36, 37-44 (2008).
- Aboushanab, T.S. & AlSanad, S. Cupping Therapy: An Overview from a Modern Medicine Perspective. Journal of acupuncture and meridian studies 11, 83-87 (2018).
- Cramer, H. et al. Randomized controlled trial of pulsating cupping (pneumatic pulsation therapy) for chronic neck pain. Forschende Komplementarmedizin 18, 327-334 (2011).
- Bier, A.K.G. & Blech, G.M. Hyperemia as a therapeutic agent. (A. Robertson & co., Chicago,; 1905).
- Brem, M.H., Bail, H.J. & Biber, R. Value of incisional negative pressure wound therapy in orthopaedic surgery. International wound journal 11 Suppl 1, 3-5 (2014).
- Karlakki, S. et al. Negative pressure wound therapy for management of the surgical incision in orthopaedic surgery: A review of evidence and mechanisms for an emerging indication. Bone & joint research 2, 276-284 (2013).
- Robert, N. Negative pressure wound therapy in orthopaedic surgery. Orthopaedics & traumatology, surgery & research : OTSR 103, S99-S103 (2017).
- Meng, X.W. et al. Wet Cupping Therapy Improves Local Blood Perfusion and Analgesic Effects in Patients with Nerve-Root Type Cervical Spondylosis. Chinese journal of integrative medicine 24, 830-834 (2018).
- Tham, L.M., Lee, H.P. & Lu, C. Cupping: from a biomechanical perspective. Journal of biomechanics 39, 2183-2193 (2006).
- Cao, H., Li, X. & Liu, J. An updated review of the efficacy of cupping therapy. PloS one 7, e31793 (2012).